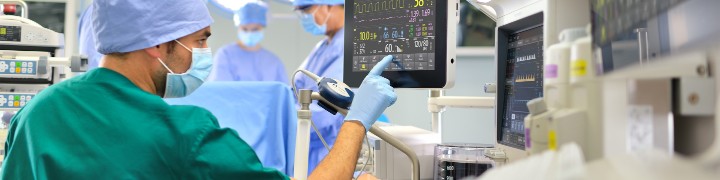
COVID-19 has caused unprecedented disruptions to the healthcare sector. Since the pandemic hit, hospitals and providers have had to deal with a surge in very sick, high-intensity patients while also having to shut down a huge portion of their traditional business. As non-urgent visits and procedures were cancelled, overall surgeries and hospital admissions plummeted. The combination of lower patient volumes, cancelled elective procedures, and higher expenses tied to the pandemic have created a financial crunch for hospitals, which are expected to lose $323 billion this year, according to a report from the American Hospital Association.
These drastic developments come at a time when the healthcare industry is already grappling with challenges posed by the digital transformation happening around electronic health record (EHR) implementation, Meaningful Use (MU) standards, HIPAA compliance, and the CMS’s Interoperability and Patient Access rule. The result is a reckoning throughout the country’s healthcare infrastructure, with a need for rapid changes and new thinking.
Everybody might be in the red right now, says RED Team member John Winenger, a veteran healthcare executive. “But how much is going to come back is the big question that everybody’s rapidly trying to assess.”
We spoke to Winenger and Michael Kreitzer, an expert hospital Interim CIO, about the biggest challenges providers and hospitals are facing, where healthcare goes from here, and the moves organizations can make—including bringing in outside help—to get out of the red and back into the black.
The Good News: V-Shaped Healthcare Recovery in Process
Healthcare was one of the sectors hardest-hit by COVID-19. But it is on track to return to pre-pandemic normals relatively quickly.
Outpatient surgeries fell by as much as 90% and hospital admissions dropped by nearly 60%, reports Healthcare Dive, citing S&P data. Fortunately, a V-shaped recovery has seen hospital admissions return to within 10% of pre-COVID levels, while outpatient surgeries have for the most part returned to normal levels.
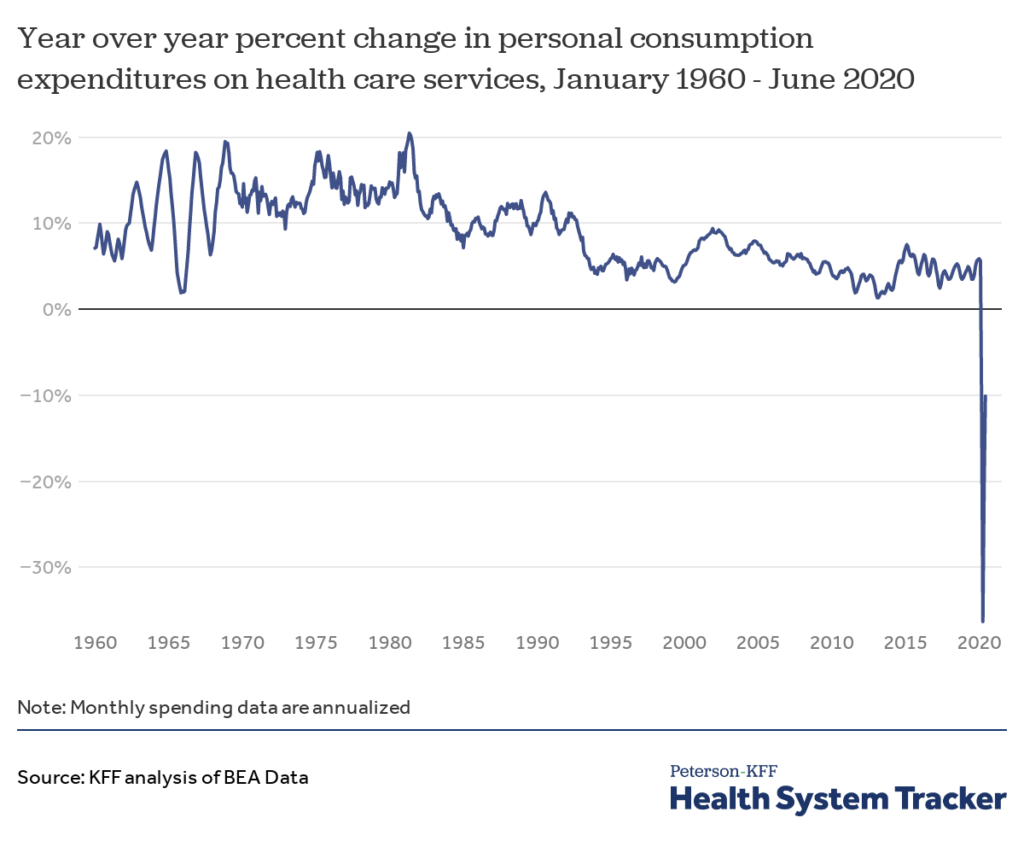
S&P predicts that the worst of the pandemic has passed for the healthcare sector and expects hospitals to fully recover by the end of 2021. Some facets of healthcare delivery, such as outpatient surgical centers, physical therapy, home healthcare and dental services, may not fully bounce back until the end of 2022, says S&P.
Winenger, however, cautions that the dust has not yet settled on the fallout from the pandemic. “I think we’re in a three to six month window with regards to how bad the hemorrhaging is going to be, but contingency plans are getting developed based on how bad the damage has been and how much bailing needs to occur to get us back into a positive budget situation,” says Winenger. “The healthcare sector is dependent on capital and without a return on investment and without healthy budgets people are not going to be spending capital.”
Current Healthcare Issues
A strong recovery notwithstanding, hospitals and healthcare providers have plenty to keep them up at night.
Even before COVID-19, industry experts expected significant changes to shake up the healthcare landscape in the years ahead. These include a shift in healthcare delivery from inpatient to outpatient settings, reducing the cost of delivering care, the consumerization of healthcare, technological advances, and protecting the privacy of healthcare data. If there’s a silver lining to the pandemic for hospitals and providers, it’s that it’s making many aspects of healthcare’s inevitable future — what some have called a “healthcare revolution” — a reality now.
Restructuring of Cost Within Healthcare Organizations
Winenger, who has served as Interim CEO for organizations ranging from hospitals to orthopedic practices, notes that unless patients are really, really sick, they are not currently coming to the hospital amid COVID-19. And the patients that are in the hospital tend to be acutely ill at numbers that hospitals are not used to.
“With higher acuity, higher staffing, and lower census, your cost per unit is going to be skyrocketing, and reimbursement is not necessarily going to be increasing to cover that cost,” Winenger says.
This poses big challenges for boards and management teams. Over the next 6 to 12 months, as organizations work on their budgets, they’ll need to figure out how to restructure costs, get fixed costs out of the system, and transfer systems of care over to telemedicine or less expensive systems.
A large proportion of a hospital’s budget goes towards fixed overhead expenses (e.g. buildings, salaries, and equipment) and not towards patient care. Unlike variable costs like medication and supplies that change based on the number and acuity of patients treated, fixed costs mostly remain the same, regardless of annual hospital census. This high ratio of fixed-to-variable costs is problematic for hospitals when they are faced with reduced admissions.
Creative cost-cutting techniques have long been a challenge for hospital executives. Traditional management strategies for adjusting fixed costs have focused on trimming administrative expenses, reducing the hours of auxiliary healthcare personnel, partnering with other practices, outsourcing services like lab work and radiology, utilizing business infrastructure service companies, and various “green” initiatives that save energy and resources.
Telemedicine is not only allowing providers to reimagine how care is delivered. It is also, along with increased telecommuting, providing opportunities for hospitals to rethink their real estate footprints. U.S. hospitals own an estimated $1 trillion worth of real estate. Chris Jennings, a policy consultant and former health care adviser to the Obama and Clinton administrations, told STAT that COVID-19 has accelerated telemedicine “by a decade.” McKinsey forecasts that up to $250 billion of current U.S. healthcare spend could potentially be virtualized.
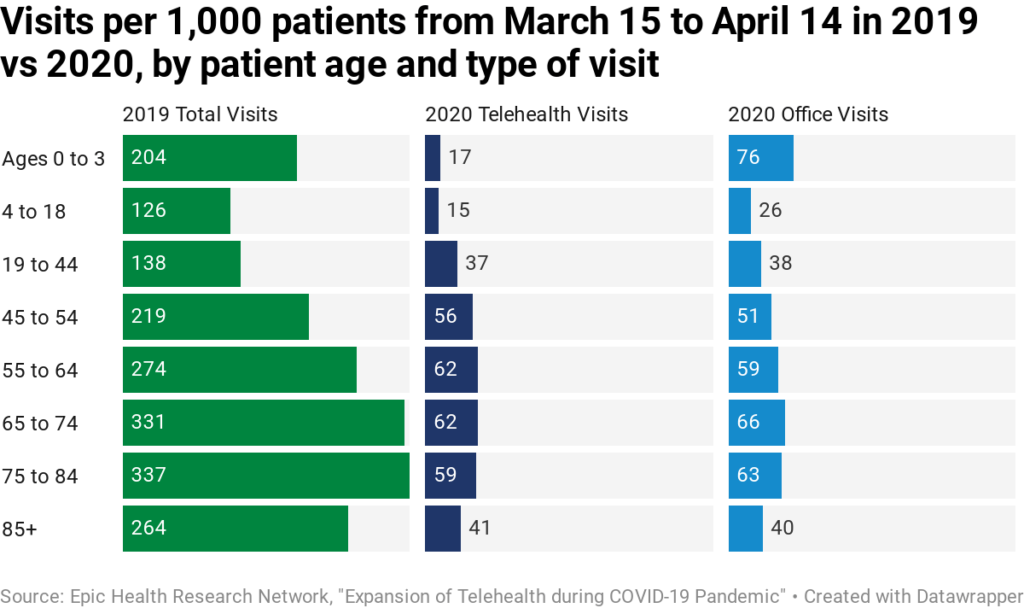
The booms in virtual care and work from home mean that hospital executives can focus cost-cutting efforts on more efficient use of operating rooms, physician offices, and administrative buildings instead of workforce reduction.
The Shift from Inpatient to Outpatient Care
Many hospitals have seen during COVID-19 that inpatient capacity is much greater than what is actually needed.
In addition to being cheaper for patients, outpatient procedures may have a higher percent of charges reimbursed by insurance carriers than inpatient procedures. Reducing inpatient bed capacity also gives hospitals more flexibility for reallocating resources.
“I think this whole [COVID-19] experience has told CEOs that they have to rapidly change their vision for where we need to be in 2030 and that is going to be focused on the outpatient, helping doctors deliver services in the outpatient setting, helping doctors with population health, providing doctors with support staff in their practices to manage care. But it’s not going to be inpatient,” says Winenger.
At the same time, cautions Kreitzer, there is a need to preserve some inpatient capacity. “We have to be able to have the flexibility to reopen previously closed patient towers because of the next pandemic,” says Kreitzer.
Technology Transformation in Healthcare
Immediate and near-term cost considerations might be foremost on the minds of healthcare executives right now, but focusing on them exclusively at the expense of medium and longer-term goals could prove disastrous.
CMS Guidance and Regulations
Hospitals and health systems have been laying off internet technology (IT) workers in 2020 due to restructuring, lost revenue during the pandemic, and outsourcing. They may find it more difficult to pull off healthcare’s digital revolution with downsized IT departments—nevermind keeping up with day-to-day tech issues.
“Not having a full IT full staff and just trying to keep their heads above water, that’s another challenge,” says Kreitzer. “CMS has not stopped issuing guidance and regulations and instructions to upgrade their IT systems, such as interoperability and patient notification. Hospitals still have to do that by early next year. And I don’t know if all of them can do that.”
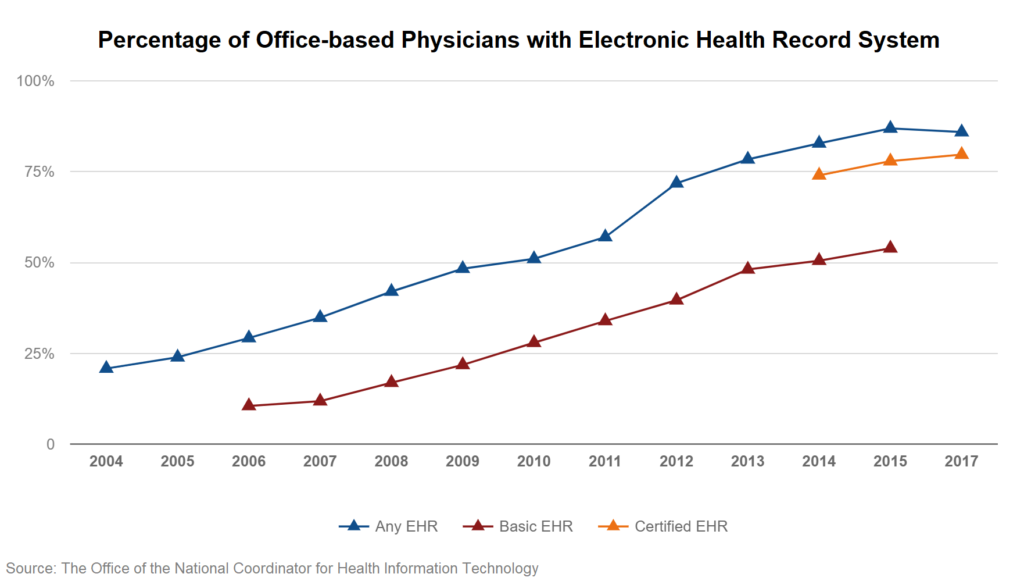
Electronic Medical Record (EMR) Implementation
Another area that requires a significant amount of hospital IT resources is EMR implementation. As records go digital, a whole new wave of concerns arise around HIPAA and Meaningful Use, both of which have risk management considerations, including cybersecurity. Failure to perform risk assessments can result in potential civil and criminal liability and disqualify an organization from receiving federal money under the Medicare or Medicaid EMR programs.
Typically, an outside expert is brought in to advise on risk assessment and risk management. An interim executive well-versed in HIPAA law, data security, and IT and can advise on encryption, levels of security and access, testing system vulnerabilities, ways to limit internal access, and related issues.
IT Disaster Recovery and Business Continuity
In the past, IT disaster recovery for a hospital or healthcare provider focused on what to do in the event of a fire or flood in the computer room or patient tower. These risks are very real. Kreitzer says that in fifteen stints as an Interim CIO, he’s been through three fires and one flood.
Modern disaster recovery, though, is broader and covers electronic data loss or corruption from hardware failure, human error, hacking, or malware. It is essential to have a plan for data backup and restoration of electronic information to ensure continuity of operations.
“How do we prepare IT’s customers?” says Kreitzer, deliberately using the word “customer” rather than “user.” “How do we prepare IT’s customers to participate in disaster recovery planning, testing, and then be ready for execution?”
Issues around disaster recovery and business continuity are typically flagged as an issue in an annual external audit report, but Kreitzer says the problem is that most organizations don’t do anything about it.
Healthcare Succession Planning
Most boards require some succession planning for the CEO if they retire or leave for other reasons. But Kreitzer says there’s not much succession planning for the rest of the executive suite.
Healthcare’s growing complexities have led to a deeper leadership structure. Today, there are dozens of hospital and health system C-suite executive positions, from the traditional CEO, COO, and CFO, to CIO (that is, Chief Integration Officer), CXO (Chief Experience Officer), and CCO (Chief Compliance Officer).
“It’s not only identifying that COO or the Chief Nursing Officer who’s next in line for the CEO. That’s the easy part,” says Kreitzer. “The hard part is, how do you prepare that person to quickly and without any balls being dropped step into that role? Succession planning is not only identification in my mind. It’s also preparation and training and mentoring.”
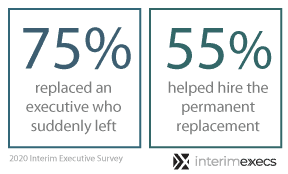
The need for interim management is often prompted by the departure of a full-time executive, and many interims take a hands-on approach to finding and onboarding the next permanent hire. Of the 600+ executives who participated in our 2020 Interim Executives Survey, 75% reported having replaced an executive that left suddenly. More than 50% said they aided in the process of hiring their own permanent replacement. Kreitzer told us in a previous interview that one of an interim’s primary duties is to create a strong foundation for the next permanent executive.
Signs You Might Need a Healthcare Interim Executive
For healthcare executives, the moment belongs to those who can meet the industry’s biggest challenges head-on. If current leadership cannot swiftly navigate the trends that are roiling healthcare, organizations can find themselves unraveling.
“The objective of execs is to figure out how to say yes and get it done,” says Kreitzer. “It may not be exactly what was asked for, but as long as you set expectations, have a good plan, have a good organization, have credibility, I think that an exec can succeed. But once they don’t succeed a couple of times, they’ve lost their credibility, and I think that they’re on a very short leash.”
When asked about the warning signs that show an interim executive may be needed, Kreitzer and Winenger gave the following perspectives.
Poor Data Management
There’s a disconnect in healthcare between the amount of data available, and how to effectively use that data. Solutions are likely buried somewhere in the data lake. The bigger problem is removing the noise and identifying the information that’s relevant to the question being asked.
A major red flag, according to Winenger, is organizations that do not have their data organized in a usable format. “If they don’t have operational, clinical, and financial scorecards prepared across all departments, and if they don’t have a good feel for their performance metrics, I think they’re going to be in a real hurt,” says Winenger. “With the huge fluctuations they’re seeing in volumes and costs, it’s going to be difficult to assess exactly where to start to fix it.”
An interim CIO can help to figure out, from an EMR data management perspective, whether a hospital or healthcare provider has the right reporting available.
“Inevitably, the issues are IT management foundational methodologies not in place,” says Kreitzer. “Methodologies that should have been in place many generations ago are not in place like basic project management. There should be a clear plan and way to track status against that plan.”
Financial House Is On Fire
Organizations might assess their fiscal year in terms of how they did relative to their goals and planning. Obviously, due to COVID-19, nobody is where they thought they would be. Forecasting through the ongoing uncertainty is going to be extremely difficult as well, but that’s no excuse for the CEO not to have a plan.
“Just reporting bad news is not good enough. What are you going to do about it?” says Kreitzer, adding that the ones who can figure out how to minimize the blow and set a clear plan forward are the ones who are going to survive and maybe even thrive years from now.
Interim executives put together a plan to rapidly stabilize an organization or turn around something that isn’t working well. Winenger believes that we are in a time when many governing boards are fearful and hesitant because of the rapid change that needs to occur.
“Those that work in this interim world, we’re very accustomed to reading the tea leaves and putting plans together pretty rapidly for improvement and helping people deal with the change process,” says Winenger. “The interim exec group has very good instincts on how businesses need to run and what change needs to occur.”
Interims and Your Leadership Team
Winenger and Kreitzer outlined a typical action plan for their interim assignments that begins with what John calls a 1 -2 week “listening tour.” After they put their ear to the ground and gather feedback from across the company, they have a plan to get the organization back on track–usually within a month.
“All of my work seems to be rooted in coming and doing a listening tour very rapidly. Having some crucial conversations before you get in the door but coming in and having a plan developed to either turn around something that’s not working well or to get a plan rapidly assembled and deployed to get things stabilized,” says Winenger. “Within 30 days, I’ve got a straw model of a turnaround plan and a work plan to achieve the goals.”
Part of that plan is how the interim works with an existing leadership team to assess and drive change. Kreitzer says that an interim has to ask, “Do I have the skillsets sitting around the table to get me where I need to be?” Unfortunately, that is not always the case. “People want to believe that the existing people in the existing leadership positions can come along for the ride and make the changes, but the reality is they are not all going to be able to make that journey,” says Winenger. “Sometimes we can bring about change without losing folks, but sometimes we can’t.”
InterimExecs RED Team is an elite group of CEOs, CFOs, COOs, and CIOs who help organizations through turnaround, growth (merger, acquisitions, ERP/CRM implementation, process improvement), or absence of leadership. Learn more about InterimExecs RED Team at www.interimexecs.com/red-team or call +1 (847) 849-2800.
More Resources:
*An Interim CFO Brings Financial Stability & Profitability To Healthcare Providers
*Healthcare’s Next Stand: Patients Must Become Consumers